No matter how good a physician you are complications happen. In a perfect world, you’d be able to prevent them all, but until that time, one of the best things you can do is be prepared for when one arises. How better to prepare than to learn from the experiences of some of the best?
At Cosmetic Surgery Forum, we always encourage honest and open dialogue – and talking about complications is no exception. In this article, get a peek at the transparency you’ll see in all of our sessions as, in their own words, CSF contributors and faculty share their advice for managing complications.
Featured Contributors: Drs. Jeanine Downie, Hassan Galadari, Sahar Ghannam, Joe Niamtu, Joel Schlessinger, and Amy Taub
A Few Cases
A Comprehensive Treatment Plan
Jeanine Downie, MD – Montclair, NJ
Several years ago now, I had a bad Radiesse complication.
It was a branch of the angular artery that was occluded, I flipped open the mouth of the individual and cut where the blockage was. Half of his face pinked up instantly. So obviously knowing your anatomy is very helpful.
Besides this, I used antibiotics, Nitropaste, Vitrase and saline flushes. Then the arterial vasodilator Viagra was used. The patient had 10 treatments or so with the hyperbaric oxygen chamber and Fraxel was used for improved texture, as well as the Excel V laser for telangiectatic areas. Fortunately, I was able to get his face to return to baseline.
It was a difficult experience and my best advice is to make sure that you give the patient your cell phone number, contact them morning and evening at the bare minimum and even go over their house if you need to do so. They need to know that you are in their corner and will work with them through this and that it is your complication with them—not just their complication.
Clear communication about what the course will be and how long it may take is also essential.
Complications are never easy, but with good patient management skills we doctors can get through the tough times.
Address it Immediately
Hassan, Galadari, MD – Al Ain, United Arab Emirates
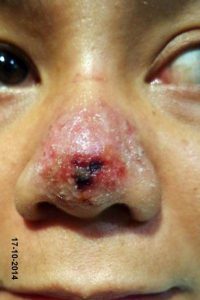
I had a patient who was seen by a visiting doctor in a clinic and her nose was injected with an HA filler. After injection, the doctor immediately traveled. The patient complained of pain later during the day, called the clinic and was told that the doctor was not there anymore and will not be there till the month after. They would not direct her to anyone else and she was informed that the pain would subside with time. The next day, the patient complained of even more pain and she started noticing change in color of the affected area. She called the clinic again and she was seen by the family doctor who owns the clinic. She was told that this was beyond their expertise and they cannot reach the doctor who injected her. They gave her some painkillers and some arnica cream to help the bruise. The condition worsened and finally the patient decided to see me in clinic. At that point, it was a few days off and the involved area had already developed epidermal breakdown and necrosis.
When the patient came to me, I immediately injected hyalase (PDF) and started her on aspirin. It was important for us to try to avoid as much scarring as possible, which was impending given the degree of epidermal breakdown that she had on presentation. With proper wound care and emollients, she healed very well with minimal scarring, which was still slightly apparent. She was happy enough with the results that she did not seem interested in trying any laser treatments to help further improve the scarring.


Keep a Close Eye on the Situation
Sahar Ghannam, MD PhD – Alexandria, Egypt
Vascular compromise and complications due to fillers are the nightmare of anybody who injects.
I know it is controversial, but as I am preparing to inject, I have the help of my nurse to keep her eyes on the injection site and the syringe. I always pull on the plunger withdraw and wait a few seconds. If she sees blood, she will tell me, “you are in!” I then withdraw the needle, get the syringe behind the chair where the patient is (the patient should not see it, of course) and I re-prepare the syringe again.
In one instant, it was the last bit in the syringe and I actually injected after there was blood in the syringe. The area became blanched and swollen immediately (of course). So I said to the patient that, in order to avoid a big bruise, I am going to inject something else. While my staff was preparing the hyaluronidase and getting hot towels, I was pressing firm on the area.
I injected the hyaluronidase, held the warm compress and asked the patient to wait for an hour. When she left the office, the blanching was gone, though she was still swollen and had some erythematous. We instructed the patient to take a selfie that night and send it to the office. The patient reported vascular compromise hours after the injection. We asked that she come in the next day. The problem was resolved with no additional treatment needed during the follow-up. The patient was happy, as, of course, was I.
I think the key was to remain calm and not panic. This kept the patient calm, as well, and allowed us to handle things smoothly.
Turn it Around and Provide Additional Value
Joel Schlessinger, MD – Omaha, NE
Whenever I have a complication I embrace the opportunity to provide value for the patient, even if it isn’t a standard complication or simply dissatisfaction from the patient. This often defuses the issue and leaves us with a lifelong patient.
Recently, we had a patient who felt that the Botox we injected left her with droopy brows. Despite the fact that we always tell patients they won’t be able to lift their eyes after it, she was still expecting to be able to do this. At the time of the appointment we offered her a free Ultherapy for the brow area (normally a $1000 procedure) for free. She was delighted and left signing our praises.
It’s not always possible to convince an unhappy patient to come in, but we are usually successful and that allows a conversation to happen and can save a relationship.
Tips and Suggestions
Follow-up Procedure Tips
Amy Taub, MD – Chicago, IL
If there is a divot from a kenalog injection or a shave removal, I find microneedling at a depth of 2.5 mm until uniform superficial bleeding once a month for 3-5 months to be incredibly helpful in resolution.
Also, if anybody gets “stripes” from IPL, I have found that performing thulium 1927 over the area resolves it more quickly and better than doing more IPL.
Learn from the Experience
Joe Niamtu, DMD – Midlothian, VA
Embrace your complications as they can make you better and help teach others how to avoid them. I meticulously document significant complications with photos, video and follow-up data. I give a great complications lecture, not because I have so many, but because of my meticulous documentation and honesty. Some surgeons deny having complications because they let their ego get in the way of education. All surgeons will have complications. They are an inevitable part of surgery. Very busy surgeons will probably see more complications than surgeons that perform less surgery just from sheer volume. Many lawsuits arise from complications, not from the actual complication, but from how it was handled by the surgeon and staff. Some tips on managing them include:
- Have an exhaustive informed consent process with written, verbal and video consents.
- Don’t downplay possible complications. Blindness, stroke or even death can occur with some of the most benign cosmetic procedures. Tell it like it is.
- Tell patients up front in the pre-op process that although complications are rare they can occur and if they do, you will shepherd them through the healing process and stand by them.
- Don’t operate on patients that are overly concerned about complications.
- Having meticulous documentation of another patient’s complication with photos of progress can allay the fear of someone who has necrosis or nerve weakness. Knowing it has happened to
- others and they healed is very reassuring.
- Do something or refer them to someone who can. Patients get very antsy when “nothing is done.”
- Don’t be defensive or try to blame the patient. Be caring and contrite and refer if you are not confident of the treatment.
- Treat these patients with special attention. Assign your most caring and communicative staff member to this patient and have them in the room at every appointment to help bond. A caring
- staff person can deflect animosity towards the surgeon.
- Never rush these patients. See them when you have time. The end of the day is best when no one else is in the office and you can devote 100% to them.
- If a patient wants a refund, you should probably do it, but never without a legal release. What you lose in refund may be 10 times less than the time out of the office for depositions or court.
- Stick with procedures that you are proficient with and avoid those that cause problems in your practice.



Leave a Comment